Southern Iowa Mental Health Center (SIMHC) is seeking new board members to guide its mission and development in being the best mental health treatment facility in the area. SIMHC is a Community Mental Health Center and is committed to providing high quality mental health care to any and all patients, regardless of their ability to pay or their stage of change. The SIMHC Board meets roughly 9 times per year and oversees the fiscal operations of the Center. SIMHC is a designated Community Mental Health Center for: Davis, Wapello, Mahaska, Keokuk and Van Buren Counties. SIMHC is actively seeking applicants from counties other than Wapello. Zoom attendance to meetings is permissible. Please complete the application below and submit to: Simhc@SimhcOttumwa.org if interested. Please call Christina at: 641-814-8730 with any questions.
Behavioral Health Counselor/Therapist
This position is a member of the clinical team whose main job function is to provide mental health services to individuals, families and groups either at the mental health center or other contracted locations within the community. Mental health services specifically include: mental health evaluations; initial assessments and individual service plans; psychotherapy and counseling; treatment plan reviews; crisis intervention/emergency; preliminary diagnostic evaluations (pre-screening); and consultation and education to patients, patient’s families, or other interested parties. Other activities may arise requiring counselor/therapist expertise and coordination for quality care of SIMHC individuals.
I. PRIMARY JOB FUNCTIONS:
1. Serve as counselor/therapist providing direct care to individuals, families, or groups either at the mental health center or other contracted community sites as determined necessary by Executive Director, or Director of Clinical Services. Meet productivity standards as set forth by the Center (currently set at 70%) and assume responsibility for quality of services rendered to individuals within budgetary guidelines.
2. Conduct and document mental health evaluations such as a preliminary diagnostic evaluation (pre-screening) upon request. Conduct and document initial assessments for psychotherapy and counseling services, gathering pertinent social history for use in making appropriate diagnosis. Develop a detailed psychiatric crisis intervention plan that includes natural supports and self-help methods with individuals who have a chronic mental illness.
3. Collaborate in creating and documenting individual service plans and subsequent treatment plan reviews. Document the individual’s progress toward goals, provision of staff supports and interventions, the individual’s response to interventions and status at each visit, and reasons for continuing or discontinuing services during or after each session in the session progress note. Maintain appropriate discharge information and follow up on missed appointments.
4. Provide emergency services to individuals consistent with Center’s program plan, policies and procedures; including crisis intervention, and/or consultation and education via telephone or in person.
5. Documentation will be completed within one week of evaluation or assessment and within 24 hours of all therapy sessions. All patient information will be confidentially maintained in the Center’s electronic medical record system, in accordance with Center policies/procedures, accreditation standards, and HIPAA guidelines. Patient information will not be released without authorized release or by court order. Prepare additional reports, as requested and authorized through signed releases.
6. Be involved with other providers and in community services including case and program consultation, mental health education, and in service training, specifically with primary care physicians, upon acquiring appropriate releases. Consult/plan as needed with staff of other agencies to assure appropriate, unduplicated services to clients and coordinate consumer referrals to other appropriate human services.
7. Participate actively in Center staff meetings for case consultation, Center program planning and quality assurance/compliance review of records. Interact with support staff as needed to facilitate claim preparation for third party reimbursement and quality client care.
8. Comply with Center employee handbook and policies and procedures. Keep records of time used and submit monthly expense claims/travel reports and appropriate forms for vacation or absence, according to Center policies and procedures.
9. Maintain continuing education requirements by attending professional courses and seminars as required by licensing board to maintain license, knowledge, and professional growth.
10. May be charged with developing, coordinating and evaluating a specific program or service to the Center, including, but not limited to, grant writing, data collection, participating in utilization and risk management activities, research activities, input towards SIMHC strategic plan, or other duties as assigned by the Executive Director or Director of Clinical Services.
II. QUALIFICATIONS
1. Must hold at minimum a master’s degree in a mental health field including, but not limited to: psychology, counseling and guidance, or social work from an accredited institution; and
2. Hold a current Iowa license as required by the Iowa professional licensure laws.
III. DEGREE OF SUPERVISION
1. Administrative supervision of mental health counselor/therapist by Director of Clinical Services at least monthly or on an as-needed basis.
2. Individual supervision with a qualified, licensed mental health professional will occur minimum of weekly for master’s degree non-independently licensed persons.
3. Qualified, licensed mental health professionals may clinically supervise the work of license-eligible persons if approved by Director of Clinical Services and applicable licensing board.
4. Directly responsible to the Director of Clinical Services.
V. REQUIREMENTS FOR POSITION
1. Flexibility to alter schedule as needed for client care, within established Center hours.
2. Excellent verbal and written skills with ability to practice good communication with providers, staff, and other providers.
3. Good decision- making skills and ability for critical thinking.
4. Working knowledge of current diagnostic criteria manual as approved by American Psychiatric Association.
5. Familiarity and proficiency with electronic medical record, electronic mail, and word processing preferred.
6. Hearing and visual ability which allows for necessary understanding while rendering professional services.
7. Physical ability to stand, walk, sit, type and/or move for up to 8 hours in a working shift.
8. Strong passion for improving the mental health & substance abuse care delivery system. Must have an internal desire to want to see people do better and live better.
To apply for any of these positions, or if you have any questions, please contact: Simhc@SimhcOttumwa.org
Learn MoreOutrun the Stigma – 4th Annual 5k
Join the fun and celebrate mental health awareness on Saturday, October 8th at 10:00AM!
The race starts and ends at:
Jimmy Jones Shelter,
1 Joe Lord Memorial Dr.
Ottumwa, Iowa 52501
Registration fee:
$20 in person or $25 online.
Race day packet pickup @ 9AM

Poor Sleep After Head Injury Could Point to Dementia Risk

FRIDAY, June 11, 2021 (HealthDay News) — Sleep disorders may increase the odds for dementia in survivors of traumatic brain injury, new research suggests.
The study included nearly 713,000 patients who were free of dementia when they were treated for traumatic brain injury (TBI) between 2003 and 2013. The severity of their brain injuries varied, and nearly six in 10 were men. Their median age was 44, meaning half were older, half younger.
Over a median follow-up of 52 months, about 33,000 of these patients developed dementia. Those diagnosed with a sleep disorder were 25% more likely to develop dementia, the study found. The results were similar for men and women — a sleep disorder was associated with a 26% increase in men’s dementia risk and a 23% increase among women.
“Our study’s novelty is its confirmation of sleep disorders’ association with incident dementia in both male and female patients, independently of other known dementia risks,” said lead author Dr. Tatyana Mollayeva, an associate director of the Acquired Brain Injury Research Lab at the University of Toronto, in Canada.
“We are also the first to report on the risks that sleep disorders and other factors pose separately for male and female patients with TBI,” she added in an American Academy of Sleep Medicine news release.
Mollayeva said the findings suggest a need for greater awareness of sleep disorder risk in TBI patients.
In the study, the researchers controlled for age, sex, income level, injury severity and other health problems that could affect the results.
A study abstract was recently published in an online supplement of the journal Sleep. The findings are also scheduled to be presented Sunday during a virtual meeting of the Associated Professional Sleep Societies.
More information
The American Academy of Family Physicians has more on dementia.
SOURCE: American Academy of Sleep Medicine, news release, June 8, 2021
Learn More
It’s a Myth That Promiscuous Women Have Low Self-Esteem

FRIDAY, June 11, 2021 (HealthDay News) — The old double standard lives on.
A new study finds that many people still believe — incorrectly — that women who engage in casual sex have low self-esteem. And they don’t think the same is true of men.
“We were surprised that this stereotype was so widely held,” said study first author Jaimie Arona Krems, an assistant professor of psychology at Oklahoma State University. “This stereotype was held by both women and men, liberals and conservatives, and across the spectrum in terms of people’s levels of religiosity and sexism.”
The finding was consistent in six experiments involving nearly 1,500 participants. The results were recently published in the journal Psychological Science.
In one experiment, participants were asked to make a snap judgment about an unspecified person in their mid-20s who had one-night stands, monogamous sex or no sex.
Women who had casual sex were judged as having lower self-esteem, but participants made no similar link between men’s behavior and their self-esteem.
Participants also were asked if a person who had casual sex was more likely to have been an English major or an English major with low self-esteem.
Most chose the second one, even though it was statistically less likely to be true, the researchers noted.
Even when presented with evidence to the contrary, participants’ views didn’t change.
“When we explicitly told participants that the women who had casual sex were enjoying it and were satisfied with their sexual behavior, participants still stereotyped them as having lower self-esteem than women in monogamous relationships who were unsatisfied with their sexual behavior,” Krems said in a journal news release.
Previous research has suggested that people who are viewed as having low self-esteem are less likely to get hired, elected to public office, or be sought as friends or romantic partners.
“Although not grounded in reality, the stereotype documented in this work may have harmful effects,” Krems said. “Stereotypes like this can have serious consequences in the real world.”
More information
The Mayo Clinic has more on self-esteem.
SOURCE: Psychological Science, news release, June 8, 2021
Learn More
COVID Antibody Treatment Is Safe, Effective in Transplant Patients

FRIDAY, June 11, 2021 (HealthDay News) — Antibody treatments are safe and effective for transplant patients with mild to moderate COVID-19, a new study shows.
Monoclonal antibodies help prevent the SARS-CoV-2 virus from attaching to cells, which helps block the spread of infection.
The findings are important, researchers said, because transplant patients with COVID are more likely to be severely ill or die.
“Monoclonal antibody therapy is really important for the transplant population because they are less likely to develop their own immunity,” said senior author Dr. Raymund Razonable, an infectious diseases specialist at the Mayo Clinic in Rochester, Minn. “Providing them with these antibodies helps them recover from COVID-19.”
The study included the first 73 solid organ transplant patients at the Mayo Clinic who received monoclonal antibody infusions for treatment of mild to moderate COVID-19.
Eleven patients had an emergency department visit and nine were hospitalized. None required mechanical ventilation, died or developed organ rejection, according to findings published June 10 in the journal Open Forum Infectious Diseases.
“While we expected monoclonal antibody therapy would be beneficial for patients, we were pleasantly surprised by the results,” Razonable said in a Mayo news release. “Only one patient required care in the ICU for non-COVID-19 indication, and, most importantly, there were no deaths.”
Last fall, the U.S. Food and Drug Administration authorized emergency use of the monoclonal antibody therapies bamlanivimab and casirivimab-imdevimab to treat mild to moderate COVID in patients at high risk for serious illness.
But many health care institutions hesitated to use them because their safety and effectiveness for transplant patients was unknown due to limited clinical data, Razonable said.
“It is important that these patients have early access to monoclonal antibody treatment,” Razonable said. “Our data show the outcomes for patients are better if they get infused earlier.”
More information
The American Society of Transplantation has more on COVID-19.
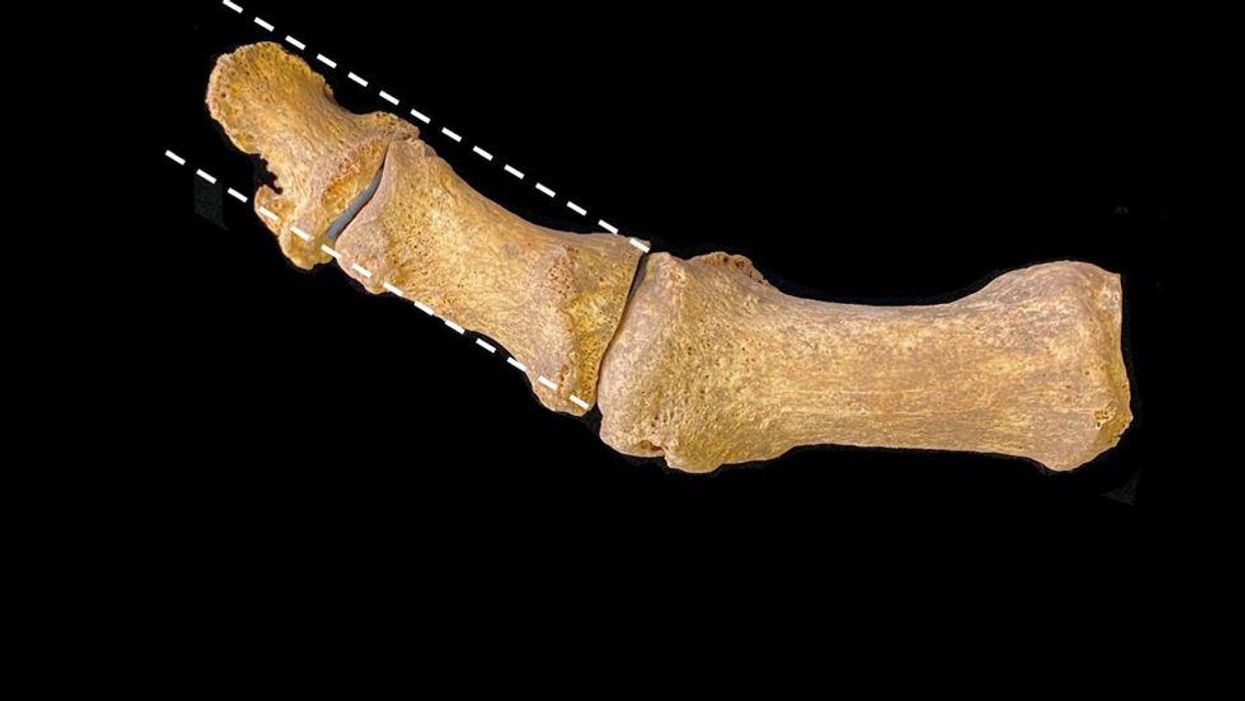
Middle Ages Misery: Medieval Shoe Trend Brought Bunions

FRIDAY, June 11, 2021 (HealthDay News) — Suffering for fashion is nothing new. Researchers in the United Kingdom have unearthed new evidence that stylish pointed shoes caused a “plague” of bunions in the late medieval period.
Investigators from the University of Cambridge analyzed 177 skeletons from cemeteries in and around the city of Cambridge. Included were a charitable hospital, the grounds of a former Augustinian friary where clergy and wealth benefactors were buried, a local parish graveyard that held the working poor and a rural burial site by a village.
Researchers inspected foot bones for the bump by the big toe that is the hallmark of hallux valgus, known to millions of sufferers as bunions.
They found that those buried in the town center, particularly in plots for wealthier citizens and clergy, were much more likely to have had bunions.
Only 3% of the rural cemetery showed signs of bunions, 10% of the parish graveyard, 23% of those on the hospital site and 43% of those at the friary.
While just 6% of individuals buried between the 11th and 13th centuries had evidence of bunions, 27% of those from the 14th and 15th centuries were hobbled by the affliction.
That’s likely because shoe style changed significantly during the 14th century, when it shifted from a functional rounded toe box to a lengthy pointed tip.
“The 14th century brought an abundance of new styles of dress and footwear in a wide range of fabrics and colors. Among these fashion trends were pointed long-toed shoes called poulaines,” said study co-author Piers Mitchell, from Cambridge’s archaeology department.
“We investigated the changes that occurred between the high and late medieval periods and realized that the increase in hallux valgus over time must have been due to the introduction of these new footwear styles,” Mitchell said in a university news release.
Hallux valgus is a minor deformity in which the largest toe becomes angled towards the second toe and a bony protrusion forms at its base, on the inside of the foot. Though genetics and muscle imbalance can predispose a person to bunions, the most common contemporary cause is restrictive boots and shoes.
In the 13th and 14th centuries, it was increasingly common for those in clerical orders in Britain to wear stylish clothes — a cause for concern among high-ranking church officials, Mitchell noted.
Across late medieval society, the pointiness of shoes became so extreme that in 1463 King Edward IV passed a law limiting toe-point length to less than 2 inches within London.
The majority of remains with signs of bunions in the study, 20 of 31, were male.
Lead author Jenna Dittmar, who conducted the work while at Cambridge, also found that skeletal remains with hallux valgus were more likely to show signs of fractures that usually result from a fall.
“Modern clinical research on patients with hallux valgus has shown that the deformity makes it harder to balance, and increases the risk of falls in older people,” Dittmar said in the release. “This would explain the higher number of healed broken bones we found in medieval skeletons with this condition.”
The paper appears in the June 10 issue of the International Journal of Paleopathology.
More information
The American College of Foot & Ankle Surgeons has more on bunions.
SOURCE: University of Cambridge, news release, June 10, 2021
Learn More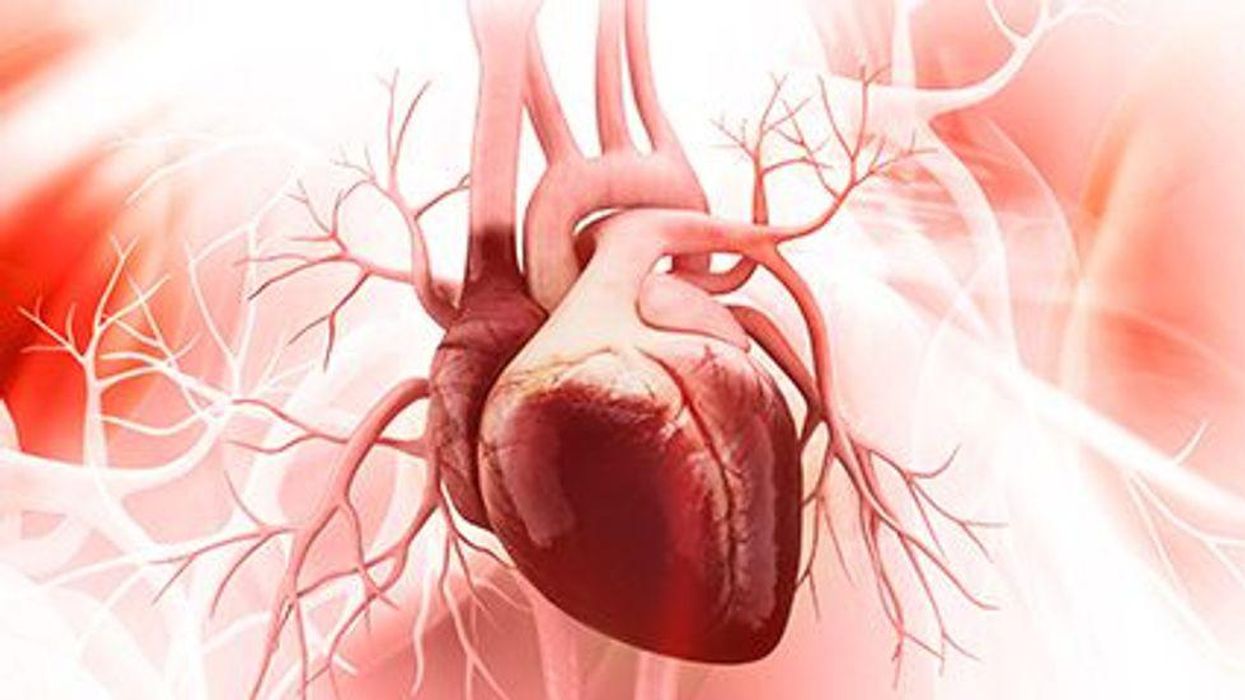
Old Age No Bar to Successful Heart Transplant, Study Finds

FRIDAY, June 11, 2021 (HealthDay News) — People over 70 are far less likely to be considered for or to receive a new heart — even though new research suggests their survival rates after transplant are similar to those of younger patients.
For the study, the researchers analyzed data on more than 57,000 adults (aged 18 and older) listed as heart transplant surgery candidates in the United States between January 2000 and August 2018, and they found that only one in 50 was aged 70 or older.
The rate was the same among the more than 37,000 patients who actually had a heart transplant during the study period. However, the researchers did find that the number of older patients receiving a heart transplant each year rose from 30 in 2000 to 132 in 2017.
There was no significant difference between age groups in death rates in the first year after heart transplant, even though older patients were more likely to receive hearts from older donors with chronic diseases, like diabetes and high blood pressure.
The difference in death rates between older and younger patients within five years after heart transplant disappeared when the researchers accounted for factors like patients’ body mass index (or BMI, which is an estimate of body fat based on weight and height) and the time patients spent on the transplant waiting list.
Older patients were more likely to have a stroke after a heart transplant, but the risk was still very low (3.5%). Most strokes in older patients occurred in the third year after their transplant, according to study author Dr. Abhishek Jaiswal, of the Hartford Hospital in Connecticut, and colleagues.
The study, published online June 8 in the Journal of the American Geriatrics Society, shows that older age alone should not prevent people from being considered for heart transplants, the researchers said.
In addition, people 70 and older with heart failure should consider asking their cardiologist if they could be a candidate for a heart transplant, the study authors suggested in a journal news release.
The researchers noted that most of the older patients in the study who received heart transplants were white, not frail, and didn’t have other chronic diseases, and that this group of patients doesn’t represent most older adults who have heart failure.
More information
The U.S. National Heart, Lung, and Blood Institute has more on heart transplantation.
SOURCE: Journal of the American Geriatrics Society, news release, June 9, 2021
Learn More
Smokers, Obese People Need Major Heart Interventions Earlier in Life

FRIDAY, June 11, 2021 (HealthDay News) — In a finding that confirms healthy habits make for healthy hearts, new research shows that smokers and obese people must have their clogged arteries cleared at much younger ages than nonsmokers or people who are a normal weight.
It found that angioplasty and/or stenting to widen coronary arteries and restore blood flow had to be performed in smokers nearly a decade sooner than in nonsmokers, and that obese patients who had these procedures were four years younger than patients who weren’t obese.
Women also typically had their first procedure to clear blocked arteries at a later age than men, according to the researchers.
The study included more than 108,000 patients without a history of heart attack who were treated at hospitals across Michigan participating in the Blue Cross Blue Shield of Michigan Cardiovascular Consortium.
Nearly all of the patients had at least one risk factor for heart trouble — including smoking, obesity, high blood pressure, high cholesterol and diabetes — and most of them had three or more risk factors.
Over the past decade, rates of obesity and diabetes have increased among patients undergoing their first angioplasty or stent procedure, while rates of smoking and high cholesterol have decreased, according to the researchers.
“Smoking is a completely preventable risk factor,” said senior study author Dr. Devraj Sukul, an interventional cardiologist and a clinical lecturer at the University of Michigan Health Frankel Cardiovascular Center.
“If we direct additional efforts at preventing smoking and obesity, we could significantly delay the onset of heart disease and the need for angioplasty and stenting,” Sukul said in a university news release.
“In Michigan, we will work to help every smoker quit at the time of cardiac care because it is an unmatched teachable moment for patients,” said Dr. Michael Englesbe, a surgeon and professor at Michigan Medicine.
The findings were published June 9 in the journal PLOS ONE.
More information
The U.S. National Library of Medicine has more on angioplasty and stent placement.
SOURCE: Michigan Medicine-University of Michigan, news release, June 9, 2021
Learn More
Houston Methodist Suspends Nearly 200 Workers Who Refuse COVID-19 Vaccines

THURSDAY, June 10, 2021 (HealthDay News) — Nearly 200 employees of the Houston Methodist hospital system in Texas have been suspended without pay for refusing to get COVID-19 vaccines.
Nearly 25,000 workers met Monday’s deadline to be fully immunized, but 178 failed to do so and were suspended, including 27 who had received one dose of a two-dose vaccine, CBS News reported. The hospital system previously warned that unvaccinated employees would be fired as of June 21.
The policy has triggered a court challenge by a group of unvaccinated workers who claimed they are being used as “human guinea pigs,” CBS News reported. But Houston Methodist said in a statement that, “It is legal for health care institutions to mandate vaccines, as we have done with the flu vaccine since 2009.”
“As the first hospital system to mandate COVID-19 vaccines, we were prepared for this,” Marc Boom, M.D., the chief executive officer of Houston Methodist, said in a statement. “As of today, several other major health care centers have followed our lead and have announced their own vaccine mandates, with many more to follow soon.”
That includes the University of Pennsylvania Health System (UPHS), which is requiring all employees be vaccinated by Sept. 1, 2021, CBS News reported. More than 33,000 of approximately 44,000 workers are fully vaccinated, UPHS said in announcing its mandate in late May.
Learn More
